
Sexual and Reproductive Health and Rights and the Post-2015 Agenda: What’s Next?

Guest post by Françoise Girard, President of the International Womens Health Coalition (IWHC)

Women’s rights advocates at the 58th session of the Commission on the Status of Women on March 21, 2014. Photo credit: UN Women/Jeca Taudte
“You’ve done remarkably well!” Those were the admiring words of an incredulous high-level United Nations (UN) official, when a colleague and I met him a few weeks ago to discuss the outcome of the Open Working Group (OWG) of the General Assembly on the Sustainable Development Goals (SDGs). “We,” of course, are the women’s groups (organized as the Women’s Major Group) who’ve fought long and hard to ensure that a standalone goal on gender equality would feature in the SDGs proposed by the OWG. The inclusion of gender equity was not a given, but it was achieved.
We had also pressed governments to ensure that sexual and reproductive health and rights (SRHR) would be included as targets under both the gender goal (SDG 5) and the goal on health (SDG 3). We came away with a significant, if partial result: Under SDG 3, governments agreed, by 2030, to “ensure universal access to sexual and reproductive health care services, including for family planning, information and education, and the integration of reproductive health into national strategies and programmes” (target 3.7). Under SDG 5, they also agreed to “ensure universal access to sexual and reproductive health and reproductive rights as agreed in accordance with the Programme of Action of the ICPD and the Beijing Platform for Action and the outcome documents of their review conferences” (target 5.6).
Governments also agreed to “eliminate all harmful practices, such as child, early and forced marriage and female genital mutilations” (target 5.3). Other important targets included to eliminate all forms of violence against all women and girls (target 5.2), reduce the global maternal mortality ratio to less than 70 per 100,000 live births (3.1), end the epidemics of AIDS, tuberculosis, and malaria (3.3) and achieve universal health coverage, including financial risk protection, access to quality essential health care services, and access to safe, effective, quality, and affordable essential medicines and vaccines (3.8). Compared to the Millennium Development Goals, the proposed SDGs represent significant progress, addressing critical areas for action that, if implemented, will transform the lives of women and girls globally. They also put the lie to claims that “we could never get today the agreements we obtained in the 1990s.” We have in fact gone beyond them.
What now? The General Assembly will begin its final negotiations on the final post-2015 development agenda early next year, for adoption in September 2015. Governments from the global South have clearly indicated that they expect the outcome of the OWG to be the basis for negotiation, and would not tolerate attempts by the Secretary General’s staff to “streamline” its 17 goals and 169 targets. That is good news for SRHR, because these targets were the most thoroughly debated and negotiated in the OWG. What emerged on SRHR from the OWG certainly represents global consensus, despite objections from a handful of opponents led by the Holy See and Saudi Arabia.
The OWG document can and should be improved upon. Human rights, the rule of law, and access to justice were not sufficiently established as key aspects of development. As noted by several governments last month at the UN General Assembly’s first ever panel discussion on child marriage, preventing child, early, and forced marriage should be its own target since it has multiple, far-reaching causes and consequences. “Sexual rights” (i.e., the right of everyone to have control over matters related to their sexuality, free of coercion, discrimination, and violence) were omitted from the SDGs, despite having been agreed to by governments at Rio+20 and recent ICPD Beyond 2014 reviews in Africa, Asia-Pacific, and Latin America and the Caribbean. Non-discrimination on the basis of sexual orientation and gender identity, which the UN Human Rights Council has just again denounced, should be included. Finally, adolescents and their right to sexual and reproductive health services and information, including comprehensive sexuality education, must be addressed if the post-2015 agenda is to be relevant for the 2.4 billion children under the age of 19 alive today.
The freedom to determine what happens to our own bodies and to make decisions about sexuality, relationships, and childbearing are fundamental facets of our lives. By investing in and promoting these rights, governments can unleash the power of women and girls and transform societies.
Adolescent Sexual and Reproductive Health Key to Achieving Sustainable Development
By Suzanne Petroni, Senior Director for Gender, Population, and Development at the International Center for Research on Women (ICRW)
Last month, the global community celebrated the 20th anniversary of the International Conference on Population and Development (ICPD). The ICPD, which took place in Cairo in 1994, led to an historic agreement by 179 governments to place women—and importantly, their reproductive health—at the center of the sustainable development agenda. Five years later, while at the State Department, I served as the U.S. government’s “officer in charge” for the five-year review of the ICPD, where we exulted when the global community agreed to advance the ICPD agenda through promoting access to safe abortion, comprehensive sexuality education, and youth-friendly reproductive health services, among other critical areas.
Uganda Prioritizes Voluntary Family Planning and Charts Course for a Rights-Based Approach
Blog post by Jan Kumar, EngenderHealth/RESPOND Project
The planets have aligned in Uganda over the past few weeks for a significant shift in the country’s national family planning (FP) program that sets it on a new and ground-breaking course. From July 28-30, 2014, the Ugandan Ministry of Health (MOH)—with support from the United Nations Population Fund (UNFPA)—hosted an event titled “Accelerating social and economic transformation through universal access to voluntary family planning.” President Museveni used this opportunity to accelerate the government’s commitment to FP2020 and to voice his endorsement for FP as a means to improve maternal health, reduce poverty, and support social and economic development. The meeting paved the way for the promotion of equitable access to a wide range of quality FP services that ensure full, free, and informed choice, as well as the protection and fulfillment of human rights for all Ugandan women and couples who wish to space or limit their childbearing.
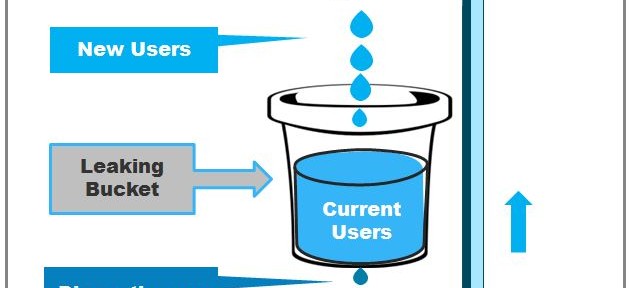
The Leaking Bucket Phenomenon in Family Planning
Guest post by Anrudh K. Jain, Ph.D., Distinguished Scholar, The Population Council
Family planning (FP) programs in developing countries have been experiencing a phenomenon that I like to call “the leaking bucket.” Let’s say that you place a bucket under an open tap and watch the water level rise, until you discover a hole in the bottom of the bucket. Water is now leaking out of the bucket. Filling the bucket will be easier once the hole is plugged. In the same way, meeting women’s desire to reduce unwanted fertility will become easier once FP programs pay more attention to contraceptive discontinuation.
Meeting the Family Planning Needs of Women and Couples Affected by HIV

Guest post by Tricia Petruney, Technical Advisor, FHI360
Like all women and men, people living with or at risk of acquiring HIV have the right to determine the number and timing of their children and to safely achieve their reproductive intentions. Yet many women and couples affected by HIV lack access to family planning (FP) services and experience disproportionately high rates of unintended pregnancy and abortion. Why is this so? One major challenge is that myths, misinformation, and stigma with regard to the sexual and reproductive health (SRH) rights of people affected by HIV continue to persist among healthcare workers.
Research has shown that healthcare providers often have poor knowledge, attitudes, and behavior with regard to providing contraception to clients affected by HIV. For example, they often (incorrectly) emphasize condoms as the sole FP option appropriate for these women and couples. Moreover, most do not routinely discuss the importance of dual method use, offer other more reliable contraceptive method options, or provide emergency contraception.
Missing Links: Sexual and Reproductive Health and Rights in the Post-2015 Global Development Agenda
On July 17, Katja Iversen, CEO of Women Deliver, published “Working Hard to Get the World We Want: Sexual and Reproductive Health and Rights After 2015” on The Huffington Post’s Global Motherhood blog. In this post, Iversen reports on the work of the Open Working Group (OWG) for Sustainable Development Goals, which is comprised of representatives from 70 countries and tasked with the creation of a new global framework for development that they are set to present to the United Nations Secretary-General Ban Ki-moon by the end of July. The influence of this report on the future of international development, sustainability, and human rights cannot be overstated.
The goals and targets it proposes—and the issues explicitly addressed—will be of utmost importance in the shaping of the post-2015 development agenda. Due to conservative push-back, Iversen decries, the current report language fails to include sexual and reproductive health and rights (SRHR), as well as the health of young people despite the fact that “the majority of governments have identified [SRHR] as a priority to get the world on a sustainable path.”
The blog post discusses the vital role that voluntary family planning and ensuring rights and contraceptive choices for women and girls play in ensuring equal opportunity, economic growth, and the development and maintenance of healthy populations. Iversen urges readers to take action and suggests ways to become involved in supporting the push for inclusion of SRHR in the forthcoming global development framework. Read this important post and join EngenderHealth, Women Deliver, and other organizations and individuals in the effort to make SRHR a priority in the post-2015 global development agenda and a reality for all.
Can 223 million women be wrong? A reflection on the status of voluntary sterilization programs

Guest post by Lynn Bakamjian
Today, as family planning (FP) programs are receiving renewed attention and resources as a result of FP2020, several important issues have risen to the top of the investment agenda. These include increasing access to quality long-acting reversible contraceptive (LARC) methods; task-shifting FP information and services to lower level health workers to address provider shortages; and scaling- up approaches that extend services, such as postpartum FP , mobile services, and increased engagement of the private sector. As programs strive to make more contraceptive choices available to reach more than 200 million women with an unmet need for FP, there is one topic that receives little attention—how to expand access, availability, acceptability and quality of permanent methods (PMs) (voluntary female sterilization and vasectomy). (more…)
Public Sector Social Franchising: The Key to Contraceptive Choice?

Guest post by Dr. Boubacar Cissé, Social Franchise Director of Marie Stopes International Mali (MSI/Mali)
A lot needs to change if we are to make contraceptive choice a reality for every woman. Public sector social franchising has the potential to unlock real change in Mali and in low income countries around the world. The term sounds complicated, but the principle is simple: leverage the country’s existing network of health facilities to maximize the contraceptive choices available to women. Mali currently has a contraceptive prevalence of nearly 10%, with long-acting and reversible and permanent methods of contraception accounting for just 0.2% of the method mix. When more family planning (FP) options are available, more individuals can meet their reproductive intention to delay, space, or limit future births.[1]
To expand access to a broader range of FP methods for women and couples, MSI/Mali and the Ministry of Health brought together 102 health clinics under the social franchise BlueStar brand. Many of these clinics already offer short-acting contraceptive options. However, when health clinics join the BlueStar social franchise network, MSI provides support to increase the range of FP methods available to include intrauterine devices (IUDs) and implants. MSI trains doctors, nurses, and midwives to provide these additional options. We also support the management of supply chains to prevent commodity stock-outs, as well as assist health facilities to raise awareness of available FP choices.
The Road to Implementation: A User’s Guide for Applying a Rights-Based Approach to Family Planning Programs

Guest post by Mariela Rodriguez, Research Associate, Futures Group
Human rights. Contraceptive choice. Access. Information. Empowerment. What do all of these things mean? How do they relate to family planning (FP)? Since the 2012 London Summit on Family Planning and the movement it initiated, FP2020, the topic of human rights and empowerment in FP has risen on the international development agenda. We know that the Summit “underscored the importance of access to contraceptives as both a right and a transformational health and development priority.”[i] But what does this mean in practice? How can FP programs turn rhetoric about rights into a reality?
The recently published Voluntary Family Planning Programs that Respect, Protect and Fulfill Human Rights: a Conceptual Framework Users’ Guide is intended for use in conjunction with the Voluntary Family Planning Programs that Respect, Protect, and Fulfill Human Rights: A Conceptual Framework, published in 2013 by Futures Group and EngenderHealth with funding from the Bill and Melinda Gates Foundation.[ii] The User’s Guide is intended for use by a wide audience spanning policymakers, program managers, health providers, rights advocates, civil society organizations, donors, technical assistance agencies, implementing organizations, and researchers. The document contains three modules to orient stakeholders to the framework and to guide the processes for using it to assess, plan or strengthen, monitor, and evaluate FP programs through a human rights lens.
MCHIP and PSI Promote Postpartum IUD to Expand Access to Family Planning for More Women

Guest post by Holly Blanchard, Senior Reproductive Health/Family Planning Advisor, Maternal and Child Health Integrated Program (MCHIP)
Access to a wide range of safe and effective contraceptive options is every woman’s human right, including those who have just given birth. Access to family planning (FP) not only enables a woman to achieve her and her partner’s desired family size, but also contributes to improved health outcomes for both women and children. However, in many low resource settings, postpartum women are offered a limited range of FP methods, if they are counseled on postpartum FP (PPFP) at all. With increasing numbers of women delivering in health facilities, the opportunity to offer the option of immediate postpartum intrauterine device (PPIUD) services should be maximized.








